
Blue sclera is a common sign of iron deficiency in children and adults. It is characterized by a blue-tinted appearance of the sclera of the eye.
The sclera is the fibrous, white tissue that covers the eyeball. It extends from the cornea to the optic nerves in the back of the eye (see illustration below).
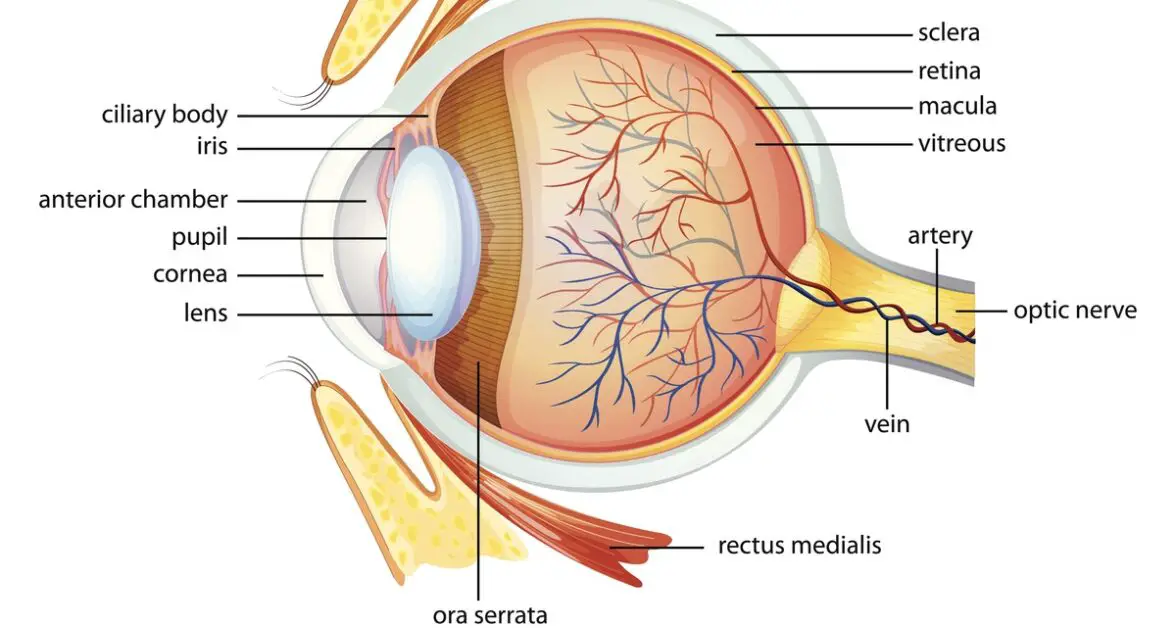
This article walks you through what you need to know about blue sclera as a sign associated with iron deficiency and anemia.
We cite recent peer-reviewed research studies and provide links to photos that show what blue sclera looks like (see blue sclera photos here).
We also briefly discuss other conditions associated with blue sclera and provide additional resources for readers interested in further details.
[Note: Interested readers may learn about 13 weird symptoms of iron deficiency here. You may also read about 13 types of pica here. Pica is one of many weird symptoms of iron deficiency characterized by strange cravings.]
Contents:
What is iron deficiency anemia?
Blue sclera and iron deficiency
Diagnostic value of blue sclera
–A common sign of iron deficiency (ID)
Blue sclera and iron deficiency in babies and children
–Osteogenesis imperfecta (OI) and blue sclera in children
Blue sclera and iron deficiency (ID) in women
What is iron deficiency anemia?
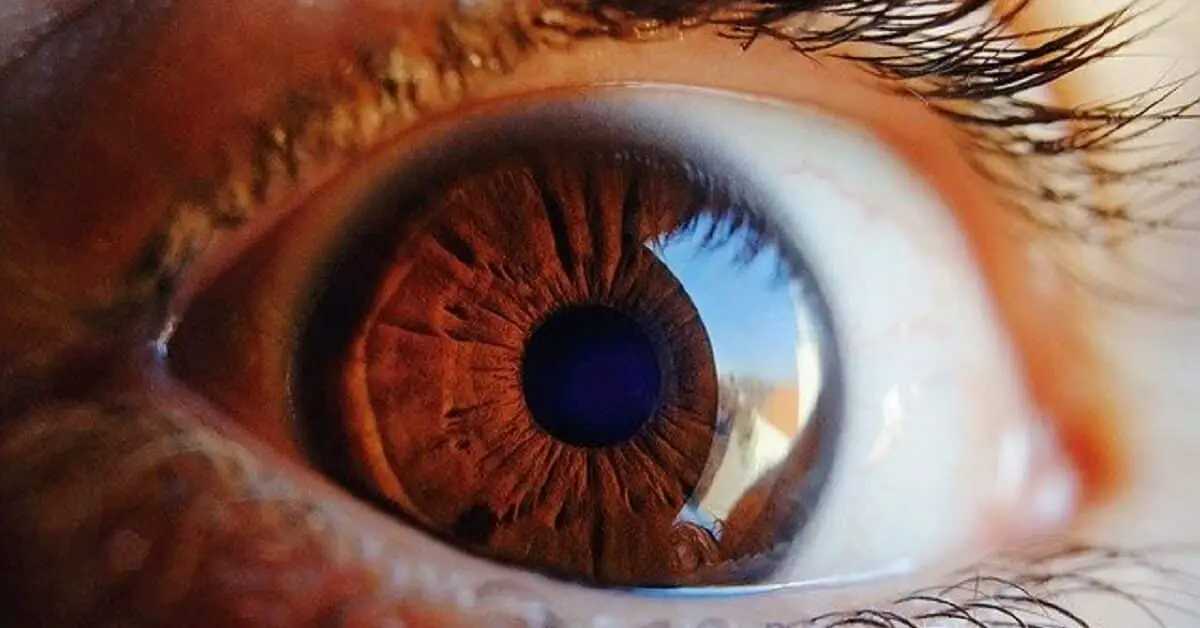
Iron deficiency (ID) is one of the most common nutritional deficiencies in the world, with more than 2 billion people affected worldwide (Viteri, 1998; McLean et al., 2009).
The prevalence of iron deficiency is high among children and pregnant women.
Mei and associates (2011) reported that the prevalence rate among pregnant women in the U.S. was 18%.
The prevalence rate increased significantly with each trimester of pregnancy, reaching as high as 29.5% in the third trimester.
A follow-up study by Mei and colleagues (2021) estimated that about 10% of U.S. children and 17% of premenopausal women suffered different degrees of iron deficiency.
Untreated iron deficiency leads to anemia (read more about iron deficiency without anemia here).
Iron deficiency anemia is when the body lacks enough iron to make healthy red blood cells to deliver oxygen to tissues and organs.
Anemia is a late-stage manifestation of iron deficiency characterized by low hemoglobin levels: ≤ 130 g/L in males and ≤120 g/L in females (Soppi, 2018).
You can have iron deficiency anemia while still having a normal full-blood count (FBC). Thus, diagnosis of the condition is based on serum ferritin levels (Soppi, 2018).
Serum ferritin is a more specific and sensitive test. It has a general cutoff of ≤30 µg/L or ≤100 µg/L in cases associated with inflammation (Lobbes et al., 2019).
Eating foods high in iron is the best way to prevent deficiency of the mineral.
Animal foods are the best sources of dietary iron.
Animal food products, such as meat, poultry, seafood, and bloodmeal, contain heme iron which has a high bioavailability (it is easily absorbed in the gut).
Plant food products, such as legumes, grains, nuts, and seeds, contain nonheme iron, which is less bioavailable (it is less easily absorbed in the gut).
However, plant sources, including herbs, may also play a role in preventing deficiency of the mineral.
Learn more about the factors that inhibit nonheme iron absorption here.
You may also learn how to enhance nonheme iron absorption here.
Blue sclera causes

Besides iron deficiency anemia, blue-tinged changes in the appearance of the sclera occur in connective tissue disorders and metabolic conditions such as:
- Liver disease
- Osteogenesis imperfecta (OI) (learn more about OI here)
- Ehlers-Danlos syndromes (EDS) (learn more about EDS here) (Hassen et al., 2017; Brooks, 2018)
According to Kumar and Shamar (2018), bilateral and unilateral blue sclera may also be associated with genetic disorders such as:
- Blue Sclera syndrome (Van der Heave Syndrome) (Alikadić-Husović and Merhemić, 2000)
- Incontinentia pigmenti
- Marfan syndrome
- Nevus depigmentosus (see also Kumar Jha et al., 2015)
Brooks (2018) identified 66 genetic syndromes, 8 health disorders, and 4 pharmacologically (medication) induced conditions associated with blue sclera (interested readers may consult the original article).
Blue sclera and iron deficiency
Several medical researchers reported that blue sclera is associated with iron deficiency in infants (Iio and Ishida, 2022), children, and adults (Hassen and colleagues, 2017).
In children and infants (older than 6 months), blue sclera may occur in acquired and congenital conditions, such as osteogenesis imperfecta (Amor et al., 2013; Mitaka, 2018) and Ehlers-Danlos syndrome (EDS).
According to Iio and Ishida (2022), in most cases, the blue tint originates in the uvea underlying the sclera. It is due to defects in collagen structure and a decrease in sclera thickness
[Note: The uvea consists of the iris, ciliary body, and choroid (see diagram below).]
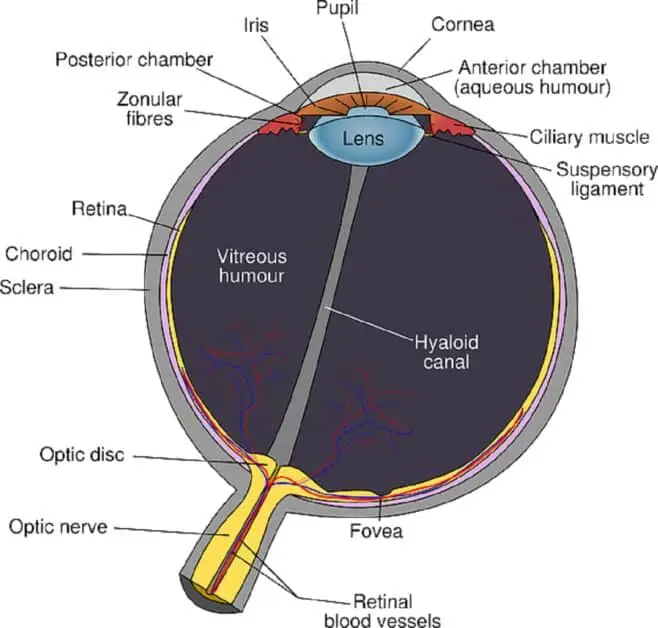
The decrease in sclera thickness makes the uvea vascularity visible through the sclera.
Is it normal in babies?
Blue sclera is common in infants younger than 6 months, according to Iio and Ishida (2022).
Blue sclera in infants younger than 6 months is due to the thinness of the sclera. However, it thickens with age (see Brooks, 2018) and becomes white in healthy infants older than 6 months.
Changes that may appear alongside a blue-tinged sclera include:
- Pallor (a pale appearance suggestive of ill-health)
- Scleral icterus (yellowing of the eyes)
Blue sclera photos
Follow the links below to view photos showing what blue sclera looks like:
Blue sclera secondary to severe iron deficiency anemia (Hassen et al., 2017)
A child with severe iron deficiency (Iio and Ishida, 2022)
Blue sclera in iron deficiency (Lobbes et al., 2019)
Osteogenesis imperfecta (Mitaka, 2018)
Diagnostic value of blue sclera

Olser (1908) was the first to report blue sclera as a condition associated with iron deficiency (via Hassen and associates, 2017).
The author reported an association between blue sclerae and iron deficiency (ID) in teenage girls (Barton and Friedman, 1990).
Kalra and colleagues (1986; 1987) confirmed Osler’s conclusion that blue sclera is predictive of ID.
A common sign of iron deficiency (ID)
Kalra and colleagues reported that blue sclera is a common sign of iron deficiency anemia in adults (Barton and Friedman, 1990; Beghetti et al., 1993).
They assessed 169 inpatients to determine the relative incidence of blue sclerae and mucosal pallor (pale mucous membranes) in patients with iron deficiency.
They concluded that the incidence of blue sclera was higher among patients with iron deficiency anemia than among patients with other types of anemia.
- Iron deficiency anemia (87%)
- Other types of anemia (7%)
- Without anemia (5.3%)
Mucosal pallor occurred in only 30% of patients with iron deficiency.
[Note: Anemia could be due to other nutritional deficiencies, such as vitamin B12 and folate. Vitamin B12 supports red blood cell formation. Pernicious anemia is a type of anemia caused by B12 deficiency.]
Kalra and associates also reported that the presence of blue sclera was not affected by age, sex, or iris color. They concluded it was a common sign predictive of iron deficiency.
They recommended checking for the eye sign during clinical examination for iron deficiency.
A strong indicator of ID
Kotsev and associates (1991) studied cases of blue sclera in adults diagnosed with iron deficiency. They concluded that blue sclera was a strong indicator of iron deficiency, with a sensitivity of 89%.
The researchers recruited 91 patients with anemia and/or blue sclerae.
Sixty-six patients had iron deficiency, of which 59 had blue sclera and 7 without the sign.
Of twenty-three patients with other forms of anemia not due to iron deficiency, only 9 had blue sclera.
Two patients without any form of anemia had blue sclera.
The researchers concluded that the presence of blue sclera was a strong indicator of iron deficiency (ID).
They recommended checking for blue sclera to identify ID and ID anemia.
Predictive value
Hassen and associates (2017) recommended that physicians consider the presence of blue sclera in adults as predictive of severe iron deficiency.
Lobbes and co-workers (2019) conducted a study to evaluate the diagnostic value of blue sclera in iron deficiency anemia.
The authors noted that although blue sclera was known to be associated with iron deficiency (ID), there were not enough studies to evaluate its specificity and sensitivity as a sign of the condition.
The researchers recruited 74 adult patients believed to have ID.
They took pictures of patients’ eyes and asked three independent physicians to grade sclera color as seen in the images. They also used computer analysis to assess the degree of the blue tint.
Out of sixty-seven patients included in the final analysis, 51 were diagnosed with ID.
The authors reported that the three independent physician’s subjective assessments of scleral color showed an association between blue color and ID.
They concluded that blue sclera had a positive predictive value for iron deficiency and that computer analysis was consistent with the clinical assessment by physicians.
They recommended that clinicians check for the sign to aid ID diagnosis because it was easy, non-invasive, and inexpensive.
Blue sclera and iron deficiency in babies and children: case studies
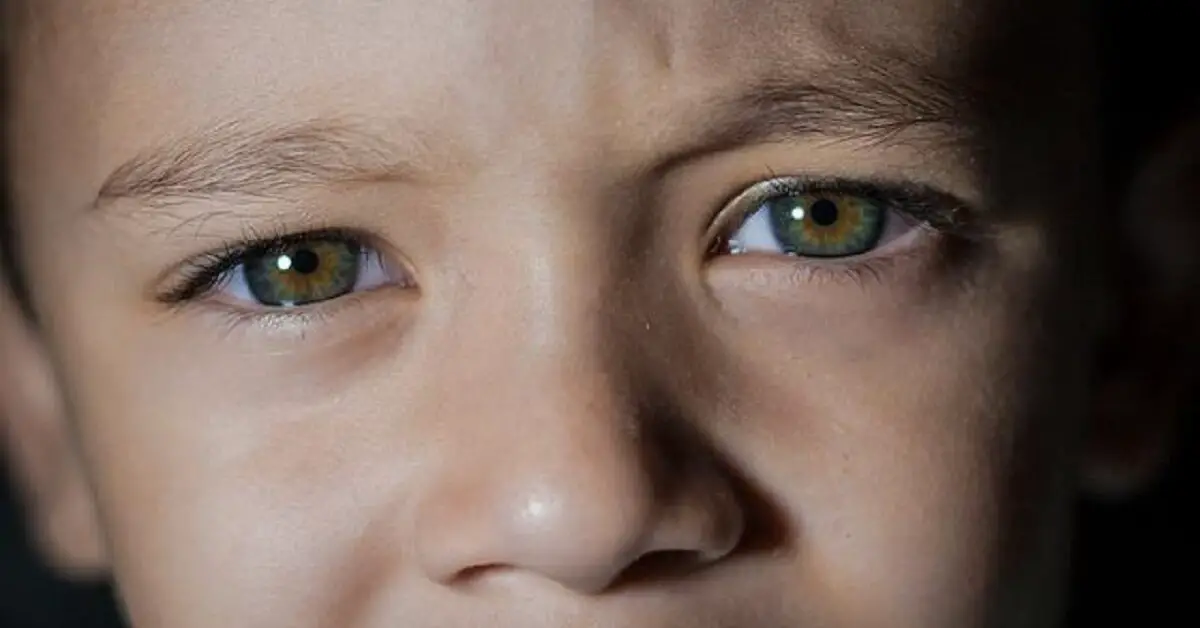
Barton and Friedman (1990) reported cases of blue sclera associated with iron deficiency anemia in babies (infants) and young children (Hassen and associates, 2017).
Case study 1
The researchers recruited 34 infants and young children aged 4 months to 5 years (25 of the children were black and 9 white) for the study.
They asked a group of pediatric physicians to confirm a diagnosis of anemia based on the following criteria:
- Children less than 2 years: Hemoglobin value less than 105 g/L
- Children older than 2 years: Hemoglobin value less than 115 g/L
- Free erythrocyte protoporphyrin value greater than 350 g/L of whole blood
The authors reported that 5 of 34 patients had blue sclera, but only two had anemia, while three patients with blue sclerae had no laboratory evidence of anemia.
The incidence of blue sclera in patients without anemia might have been because it normally occurs in infants less than 6 months.
Case study 2
Lio and Ishida (2022) reported a case involving a 12-month-old Japanese baby with normal physical and neurologic development.
The infant, who had no history of fractures suggestive of OI, engaged in ceaseless crying and cyanotic breath-holding spells (holding your breath until you turn blue).
The baby was alert and had normal body temperature, heart, and respiratory rates.
Physical examination revealed pallor (paleness) and sclera with a bluish tint.
Suspecting iron deficiency anemia, the doctors ordered blood tests that revealed microcytic anemia.
Iron deficiency is the most common cause of microcytic anemia, according to Massey, 1992.
The blood tests returned the following results:
- Hemoglobin: 6.0 g/dL
- Mean corpuscular volume: 44 fL
- Serum iron: 18 μg/dL
- Serum ferritin: 5.3 ng/mL
The doctors administered iron supplements.
At one-month follow-up, the child’s hemoglobin count had significantly increased. The color of the sclera and other signs of anemia had improved.
The authors concluded that checking for blue sclera may help physicians identify iron deficiency in children.
They added that the sign should alert physicians to the possibility of iron deficiency anemia, especially in children older than 6 months.
We shall now consider two other conditions associated with blue sclera in children.
Osteogeneis imperfecta and blue sclera in children

Blue sclera may be associated with an undiagnosed inherited connective tissue disorder called osteogenesis imperfecta (OI) OI (Mitaka, 2018).
Osteogenesis imperfecta (OI) is an inherited skeletal disorder. Patients with the condition often have low bone mass, fragility, short stature, and in some cases blue sclera (Amor et al., 2013).
Symptoms occur with various degrees of severity, ranging from mild to severe. Very mild cases may be largely asymptomatic, with patients having a normal stature and life expectancy. They may also have a slight predisposition to bone fractures.
However, severe cases may be disabling and lead to premature death.
Milder cases of OI often go underdiagnosed due to unremarkable symptoms.
According to Mitaka (2018), blue sclera is often the first and most critical sign that helps early detection of OI. Other common manifestations in undiagnosed cases may include hearing loss and severe postmenopausal osteoporosis.
Mitaka (2018) reported a case involving a 13-year-old boy diagnosed with flu. A routine physical examination revealed blue sclera and short stature.
He had a history of multiple fractures following minor injuries.
Radiological imaging showed low bone mineral density, minor bone deformity, and mild scoliosis (sideways curvature of the spine). The patient also had pectus excavatum (sunken chest bone).
Further investigations led to a diagnosis of osteogenesis imperfecta type 1.
Ehlers-Danlos syndrome (EDS)
Another condition associated with blue sclera is Ehlers-Danlos syndrome (EDS) (Roustit et al.,2019).
In EDS, the choroid layer underlying the sclera has a bluish tint.
Blue sclera and iron deficiency (ID) in women: case study

Clemente and associates (1990) conducted a study to estimate the predictive value (PV) of blue sclera in iron deficiency in women.
The study involved 498 women at a primary healthcare center.
The researchers assessed the intensity of blue discoloration of the sclera measured on a scale of 0-3.
They found that 28 of the 498 women had blue sclera, of which 21 had anemia or iron deficiency.
The researchers calculated that blue sclera had an iron deficiency predictive value of 57.14% (95% within the confidence interval of 52.77-61.51).
They concluded that blue sclera was a good indicator of iron deficiency in women. But they suggested more studies to confirm their data.
Blue sclera and ID in adults: case study

Hassen and colleagues (2017) reported a case of blue sclera involving a 54-year-old male patient who presented with a 1-week history of multiple symptoms:
- Dizziness that worsened on standing
- Generalized weakness and decreased exercise tolerance
The patient had a history of hypertension and chronic kidney disease.
He was also on medication (Aripiprazole) for mood disorder and reported having bipedal edema (swelling of both feet).
The authors reported that the patient denied experiencing symptoms, such as:
- Chest pain
- Shortness of breath,
- Abdominal pain, nausea, constipation, vomiting, diarrhea
- Abnormalities in bowel and bladder habits, dysuria, incontinence
- Palpitation
- Hematuria (blood in the urine), hematochezia (rectal bleeding), hematemesis (vomiting blood), melena (black stool)
- Weakness or numbness in the extremities
- Speech or vision changes
- Cough, fever, chills, hemoptysis (coughing up blood), hoarseness, drooling, wheezing
The authors reported that besides having blue-tinged sclera, the patient was pale-skinned and had mild jaundice.
Laboratory tests revealed the patient had severe anemia:
- Hemoglobin and hematocrit H/H: 2.8 g/dl/10%
- Iron level: 7 μg/dl,
- Blood urea nitrogen: 75 mg/dl
- Creatinine: 8.1 mg/dl
- Reticulocyte count: 1.13%
- Ferritin: 11.80 ng/ml,
- Haptoglobin: 204 mg/dl,
- Transferrin: 356 mg/dl
- Vitamin B12: 1725 pg/ml and
- Folate: 8.08 ng/ml
The doctors diagnosed severe iron deficiency anemia.
They admitted the patient to the hospital and gave him a blood transfusion. They also prescribed iron supplements.
The patient’s symptoms began improving after transfusion and iron supplements. The symptoms, including blue sclera, improved with time.

