
This article covers everything you need to know about the early warning signs and symptoms of vitamin B12 deficiency and pernicious anemia in the tongue, skin, nails, and hair.
Vitamin B12, or cobalamin, is a complex water-soluble vitamin produced by anaerobic microbes, such as Pseudomonas denitrificans, Propionibacterium freudenreichii, and aerobic microbes, such as Bacillus megaterium (Ainala et al., Chamlagain et al., Biedendieck et al.).
Ruminant animals, such as cattle, sheep, and goats, can absorb vitamin B12 produced by symbiotic bacteria resident in the rumen section of their stomach compartments. Thus, the meat and milk of herbivores are good sources of vitamin B12.
Bacteria in the human gut can also produce limited amounts of cobalamin, but it is not available for absorption by their human hosts. Humans, therefore, obtain their B12 by feeding on the flesh of ruminants.
Other animals, such as rabbits and guinea pigs, practice a form of coprophagy (poop-eating) known as cecotrophy. Rabbits can utilize cobalamin synthesized by bacteria in their guts by producing and eating a special type of soft and sticky poop known as “cecotropes” or “cecal pellets.” Cecotropes consist of partially digested food rich in vitamin B12.
In the marine world, phytoplanktons get their vitamin B12 from symbiotic bacteria. Other forms of marine life, such as fish, obtain their cobalamin by feeding on plankton. Humans may also get vitamin B12 by feeding on fish.
Cobalamin is found only in animal food products. Animals, unlike plants, use the bioactive forms of the vitamin, including adenosylcobalamin (AdoCbl or coenzyme B12) and methylcobalamin (MeCbl), as cofactors in several biochemical processes.
Methylcobalamin, for instance, is involved as a cofactor of methionine synthase in the conversion of homocysteine to methionine, a crucial step in the complex biochemical pathways involved in DNA synthesis.
B12 deficiency symptoms may occur when your body is low in the vitamin because you are not getting enough from your diet or not absorbing it efficiently from the gut.
Cobalamin plays an essential role, alongside iron and folate, in the formation of red blood cells. Inadequate supply of the vitamin may thus lead to deficiency anemia.
Anemia is a condition in which your blood has fewer than normal red blood cells (RBCs), an increased number of defective RBCs, or too low hemoglobin levels to transport oxygen to tissues and organs.
Vitamin B12 deficiency symptoms, such as fatigue, pallor, shortness of breath, dizziness, lightheadedness, irregular or fast heartbeat (tachycardia), low blood pressure, and early warning signs in the tongue, skin, nails, and hair, are due to impaired distribution of oxygen to tissues and organs.
Contents:
Pernicious anemia signs (intro)
Early warning signs in the tongue
Pernicious anemia tongue pictures
Early warning signs in the hair
Impaired B12 absorption and Intrinsic Factor
B12 absorption and achlorhydria
Vitamin B12 deficiency: What is pernicious anemia?

Although eating diets — especially strict vegan diets — low in cobalamin may cause vitamin B12 deficiency anemia, it may also be due to malabsorption of the vitamin in the gut.
Pernicious anemia (also known as Biermer’s disease or Addisonian anemia) is a type of vitamin B12 deficiency anemia caused by impaired cobalamin absorption from the ileum. Impaired absorption is due to lack of a stomach-produced glycoprotein known as intrinsic factor (IF).
Pernicious anemia is a megaloblastic macrocytic anemia characterized by increased production of defective red blood cells that are low in hemoglobin, fewer, and larger than normal. The red blood cells are unable to efficiently deliver much-needed oxygen to vital body tissues and organs.
The production of defective red blood cells in pernicious anemia is due to impaired DNA synthesis.
Vitamin B12 plays an essential role in DNA synthesis. Deficiency of the vitamin thus causes impaired DNA synthesis and consequently the disruption of formation, growth, proliferation, and maturation of blood cells in the bone marrow (hematopoiesis or hemopoiesis).
Cobalamin in its bioactive form adenosylcobalamin (coenzyme B12), also plays an active role in the production of succinyl-CoA (Krautler), an enzyme needed for the biosynthesis of the heme component of hemoglobin and myoglobin.
B12 deficiency symptoms: Pernicious anemia signs (tongue, skin, nails, hair)
Some of the early signs and symptoms of vitamin B12 deficiency and pernicious anemia are non-specific symptoms, such as:
- Pallor or pale skin
- Fatigue
- Loss of appetite
- weight loss
- Shortness of breath
- Dizziness
- Tachycardia
- Lightheadedness
Due to its role in promoting DNA synthesis, cobalamin is also involved in maintaining the health of the central nervous system (brain and spinal cord). It plays a role in the synthesis of neurotransmitters and the regeneration of nerve cells. The neurological symptoms of vitamin B12 deficiency (see list below) may, therefore, signal ongoing damage to the CNS.
- Numbness
- Pins and needles, numbness, burning sensations (paresthesia)
- Gait disturbances
- Reduced or absent reflexes
- Loss of bladder control (incontinence)
However, B12 deficiency may present with signs and symptoms in the tongue, hair, nails, and skin that may serve as early warnings or indicators of a worsening condition. You need to know these signs and symptoms and detect them early so that you can prevent the onset of more serious complications, such as irreversible neurological damage and heart diseases.
B12 deficiency symptoms: Early warning signs in the tongue
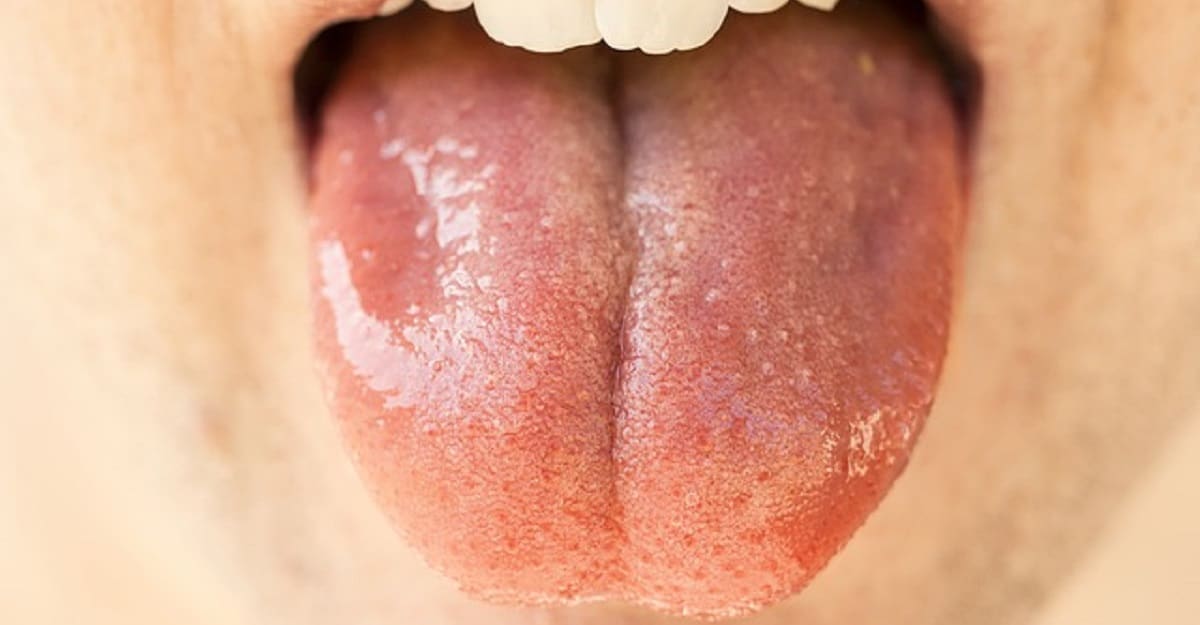
Glossitis (inflammation of the tongue) is an early indicator or “clinical marker” of vitamin B12 deficiency and pernicious anemia.
Zhou and associates concluded that for clinical purposes, the oral signs and symptoms associated with glossitis, such as “beefy red” patch, are useful early warnings (alongside low serum B12 levels <350 pg/mL) that help in the diagnosis of B12 deficiency.
According to the researchers, the oral signs and symptoms of B12 deficiency appear very early because the oral mucosa and the tongue are composed of rapidly dividing cells sensitive to cobalamin status.
Glossitis is an early warning clinical sign of vitamin B12 deficiency, according to Graells and colleagues.
Because glossitis may present with or without anemia or neurological symptoms, Graells and colleagues recommended that patients presenting with the sign need to have their vitamin B12 levels checked even in the absence of anemia.
Glossitis is characterized by swelling or inflammation of the tongue, burning sensation or pain, changes in color, texture, and appearance of the organ.
Hunter’s glossitis is a common oral sign of vitamin B12 deficiency that presents as “beefy red” patches on the tongue. If vitamin B12 deficiency is left untreated, Hunter’s glossitis may progress to atrophic glossitis (Zhou et al., Pétavy-Catala Catala et al.).
Lesions associated with Hunter’s glossitis may occur on the dorsal, ventral surfaces, and margins of the tongue. The lesions may be linear, bandlike, or irregular erythema (“beefy red” erythematous patches).
Besides the tongue, the lesions may also be found on the palate (roof of the mouth), buccal mucosa (inner lining of the cheeks), and labial mucosa (inner lining of the lips) (Zhou et al., Pontes et al.).
According to Graells and colleagues, glossitis is present in up to 25% of cases of vitamin B12 deficiency. It manifests as inflammatory changes of the tongue with bright red plaques. When left untreated, it evolves into atrophic glossitis characterized by atrophy (degeneration) of the lingual papillae.
Stoopler et al. reported the following as common features of glossitis due to vitamin B12 deficiency and pernicious anemia:
- Glossodynia or burning, painful sensation in the tongue.
- Inflamed or swollen tongue
- “Beefy red” patches on the tongue
- Pruritus (itching)
- Lingual paresthesia (feeling of burning, tingling, or prickling in the oral cavity)
- Oral lesions
- Dysgeusia (altered perception of taste in which most foods are experienced as sour, metallic, or bitter)
- Candida yeast growth on the tongue
- Reduced sense of taste
- Smooth tongue/smooth erythematous surface (due to atrophy of the lingual papillae)
The lingual papillae are structures on the upper (dorsal) surface and sides of the tongue that impart a rough texture to the organ. There are four types of lingual papillae — fungiform, filiform, vallate, and foliate.
In atrophic glossitis, the filiform and fungiform papillae on the dorsal surface of the tongue may undergo atrophy (degeneration), giving the organ a smooth appearance (Erriu et al.).
Stoopler and associates reported a case involving a 61-year-old woman who complained of burning or painful sensations on her tongue (glossodynia). Tests revealed candida yeast infection, low vitamin B12 levels, and macrocytic anemia.
Her symptoms improved after a single intramuscular injection of vitamin B12 (1000 μg), and her tongue regained normal appearance in a few days.
Lehman and associates reported a 73-year-old woman who presented with pain in the tongue (glossodynia). Physical examination revealed features of atrophic glossitis, including a “beefy red” tongue with a smooth surface. Tests revealed low serum vitamin B12 levels and macrocytosis.
The diagnosis was atrophic gastritis and pernicious anemia.
Her vitamin B12 level and symptoms partially improved after oral administration of vitamin B12 for 3 months.
Kobayashi and Iwasaki also reported a 69-year-old woman who complained of a painful tongue and reduced taste sensation lasting 4 weeks. She had a smooth and red tongue without lingual papillae (a sign of atrophic glossitis). Laboratory tests revealed macrocytosis without anemia and low serum vitamin B12 levels.
Intramuscular methylcobalamin resolved her glossitis symptoms.
Besides B12 deficiency and pernicious anemia, glossitis may also be a sign of folic acid, riboflavin (B2), and niacin (B3) deficiency (Kobayashi and Iwasaki, Reamy et al.).
Pernicious anemia tongue pictures
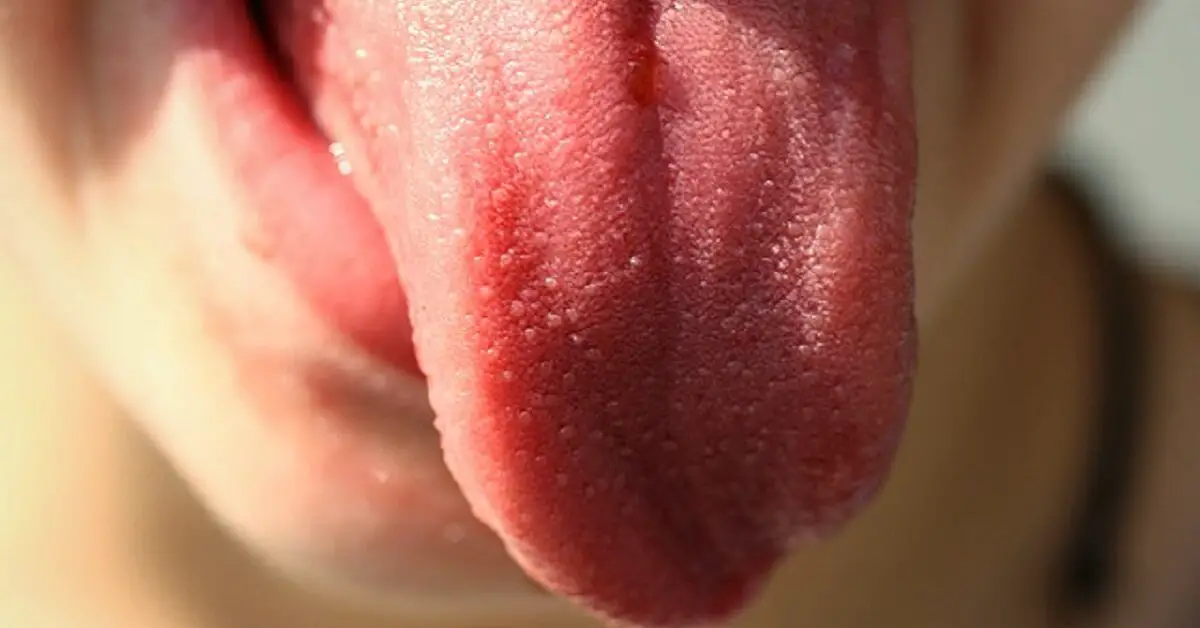
The image in the YouTube video below shows the typical “beefy red” presentation of atrophic glossitis in vitamin B12 deficiency:
This YouTube video shows what atrophic glossitis looks like.
You may view more illustrative images here: Kobayashi and Iwasaki and Stoopler et al.
Vit B12 deficiency anemia symptoms: Warning signs in the nails
Melanonychia is an early warning sign of vitamin B12 deficiency anemia that occurs in the fingernails and toenails. People with melanonychia due to cobalamin deficiency or pernicious anemia may notice a darkening of their fingernails and toenails.
The affected nails may have a dark brown discoloration. In some cases, they have a dark blue or bluish-black discoloration composed of wavy or longitudinal dark streaks (longitudinal melanonychia).
B12 supplementation may reverse this physical sign of vitamin B12 deficiency.
Afra and associates reported melanonychia in a 10-year-old boy on a strict vegetarian diet. The boy presented with bluish-black darkening or blackening of multiple fingernails and toenails. The darkening covered his entire nail plate, with deep pigmentation of the proximal nail folds and knuckles (pseudo-Hutchinson’s sign).
Blood tests revealed he had a low vitamin-B12 serum level.
His serum B12 normalized after treatment with intramuscular cyanocobalamin (1000 μg/week) for 8 weeks. There was also an improvement in his melanonychia, and the treatment continued for three months.
The authors noted that reversible melanonychia due to vitamin-B12 deficiency is more common in dark-skinned individuals.
Melanonychia is a manifestation of vitamin B12 deficiency, according to Faico-Filho and colleagues. The authors reported a 47-year-old male with a history of use of fluoxetine due to depressive disorder. The patient reported progressive hyperpigmentation of his fingernails and toenails. There was no hyperpigmentation of the skin, mucous membranes, or changes in hair color. He complained of weakness (asthenia), postprandial epigastric pain (pain in the upper abdomen after a meal), and weight loss.
Tests revealed that he had anemia and low vitamin B12 level.
The patient’s melanonychia started regressing after treatment with daily doses of 5000 μg cyanocobalamin, 100 mg pyridoxine, and 100 mg thiamine. After 3 months of treatment, the patient reported improvement in his condition. Tests also showed an improvement in hemoglobin and vitamin B12 levels.
Pernicious anemia symptoms: Early warning signs in the hair
Studies indicate that that vitamin B12 deficiency may play a role, alongside other micronutrients, such as vitamin D, folate, iron, and selenium in maintaining a healthy condition of hair.
According to Almohanna et al., cobalamin may help maintain the health of hair follicles due to its role in nucleic acid production (DNA synthesis). Thus, vitamin B12 deficiency and pernicious anemia may cause hair thinning and loss.
But although hair loss symptoms may improve with vitamin and mineral supplementation, not enough studies have been done to elucidate the exact role of B12 in hair loss conditions, such as androgenetic alopecia (male pattern baldness) and telogen effluvium (TE).
Guo and Katta suggested screening patients with hair loss for nutrient deficiency. The authors noted that nutritional deficiency may affect hair structure and growth and cause hair loss issues, such as acute telogen effluvium (TE) and diffuse alopecia.
Cobalamin deficiency may cause premature greying (also known as premature canities), according to Noppakun and Swasdikul. Treatment with intramuscular injection of cyanocobalamin reversed premature greying that occured as a symptom of vitamin B12 deficiency, the authors reported.
Premature greying may also occur in people with folic acid and biotin deficiencies (Daulatabad et al.).
Cobalamin deficiency may be associated with changes in hair color (Carmel). The researcher reported a patient with B12 deficiency whose hair color changed to a reddish hue. Supplementation triggered new hair growth that led to the restoration of normal color.
Pernicious anemia symptoms: Early warning signs in the skin
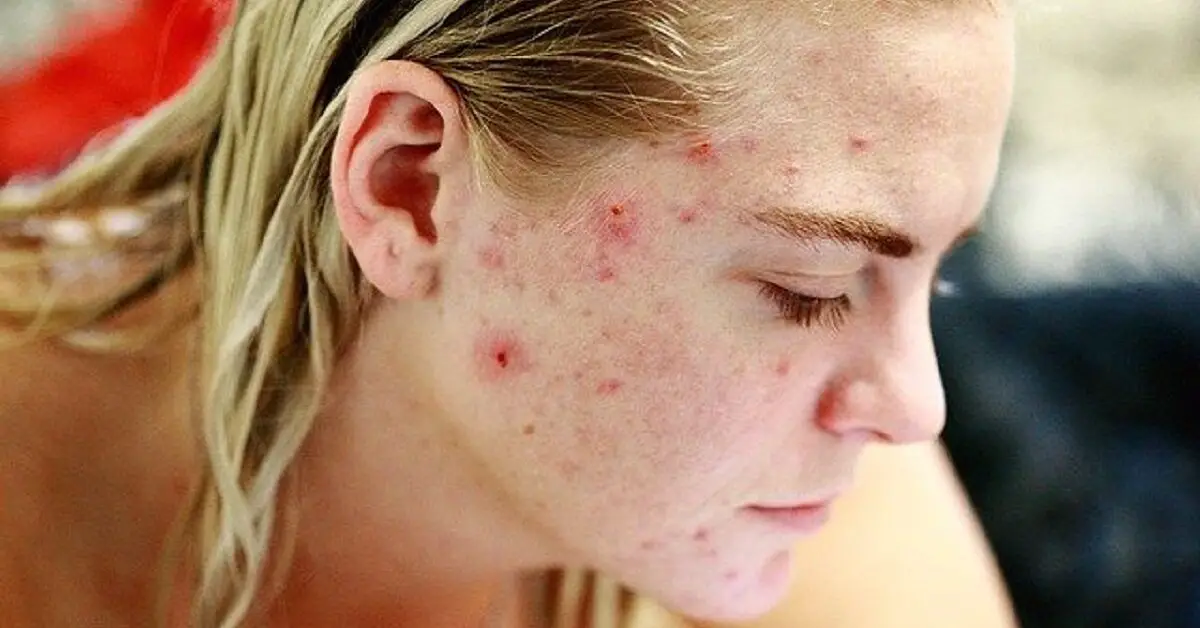
Vitamin B12 deficiency anemia and pernicious anemia are often associated with changes in skin condition, such as hyperpigmentation (Noppakun and Swasdikul).
According to Aaron et al., up to 40% of patients with vitamin B12 deficiency present with skin and mucosal changes. Kannan and associaties also reported that people with cobalamin deficiency may present with skin changes.
The authors noted that skin changes are important early warning signs and symptoms of cobalamin deficiency, but they may be overlooked because they are not specific to the condition.
Mucocutaneous lesions (skin and mucous membrane lesions that are warning signs of systemic stress, disease, or immunosuppression) may also be early warning signs of B12 deficiency. Persistent skin lesions can be a red flag sign of pernicious anemia.
Skin changes may include skin hyperpigmentation (darkening), mucocutaneous lesions, such as vitiligo (Nagarajan et al.), and recurrent angular stomatitis (lesions in the corner of the mouth also known as angular cheilitis or perleche).
Kannan and colleagues reported a nonvegetarian 34-year-old woman under care for hyperthyroidism who presented with skin lesions. The lesions were nonpruritic (no itching) and hyperpigmented macular lesions (small, dark, and flat skin lesions) distributed over the toes of both feet.
Tests revealed low vitamin B12 levels. The lesions improved after treatment with an intramuscular injection of vitamin B12 (1000 μg) and daily oral administration of vitamin B complex (B1, B6, and B12).
Agrawala and associates also reported vitamin B12 deficiency in a 35-year-female who presented with generalized weakness, weight loss, and progressive hyperpigmentation in the palms, knuckles, feet, tongue, oral mucosa, and gluteal (buttocks) region. Tests showed she had low serum levels of vitamin B12 and megaloblastic anemia due to low dietary intake.
Her skin hyperpigmentation resolved after B12 supplementation.
According to Brescoll and Daveluy, low vitamin B12 levels may be associated with dermatological (skin) changes, such as hyperpigmentation, vitiligo, aphthous stomatitis (canker sores), atopic dermatitis (eczema), and acne. Excessive levels of the vitamin may also trigger dermatological problems.
In some cases, patients with cobalt sensitivity may present with adverse dermatological reactions after B12 therapy (including cobalamin injection). Adverse reactions may include acne, rosacea, allergic site reactions, or anaphylaxis (Brescoll and Daveluy).
Pernicious anemia prevalence
Pernicious anemia is the most common form of vitamin B12 deficiency anemia among older people in developed countries.
Vitamin B12 deficiency has a higher prevalence among people older than 60 years. A survey found that B12 deficiency occurred in 6% of Americans aged over 60, compared with 3% of those aged 20-59 (Shipton and Thachil). The survey also found marginal depletion of B12 levels in 20% of Americans aged over 60, compared with 15% of Americans aged 20-59.
Cobalamin deficiency is more common among older people due to the prevalence of age-related malabsorption syndrome. In developing countries where many people subsist on a poor plant-based diet lacking in Vitamin B12, deficiency is a lifelong health issue, and symptoms of anemia may manifest in children and young adults (Allen et al.).
However, in developed countries where many people live on diets relatively high in B12-rich animal food products, vitamin B12 deficiency anemia tends to manifest later in life as pernicious anemia due to impaired absorption.
Pernicious anemia symptoms tend to manifest later in life among people on a higher plane of nutrition because the liver accumulates larger stores of the vitamin and it may take many years after age-related gut malabsorption problems start to deplete the stores.
Carmel and co-workers reported that while pernicious anemia may be a disease of the elderly whites, it appeared not to be the case in other racial groups. The authors noted a higher prevalence of pernicious anemia among younger racial minorities. The higher prevalence of pernicious anemia among younger racial minorities may be due to poorer nutrition linked with lower socioeconomic status.
Impaired B12 absorption and intrinsic factor (IF)

Impaired absorption of cobalamin (vitamin B12) in pernicious anemia is usually due to lack of a stomach-produced glycoprotein known as intrinsic factor (IF).
Intrinsic Factor (IF) facilitates the absorption of B12 by binding to it in the duodenum to form a B12-IF complex. The B12-IF complex is transported from the duodenum to the distal segment of the small intestine known as the terminal ileum, where it is absorbed.
Cobalamin is taken up into the enterocytes (the absorptive cells) of the terminal ileum after the degradation of the B12-IF complex. Once released from IF, cobalamin binds with transcobalamin II for systemic distribution or storage in the liver.
Intrinsic Factor (IF), therefore, plays an essential role in transporting cobalamin to the absorption sites in the terminal ileum. People who don’t produce enough IF are susceptible to cobalamin deficiency.
B12 absorption and achlorhydria

Impaired absorption of vitamin B12 (cobalamin) from the gut may also be due to decreased stomach acid production (achlorhydria). Most of the cobalamin ingested with food is delivered to the stomach in a protein-bound form. Stomach acid (hydrochloric acid) facilitates the separation (proteolytic cleavage) of vitamin B12 from protein after which it binds with transcobalamin I (also known as haptocorrin) for safe passage through the acidic stomach medium to the duodenum.
Stomach acid facilitates the release of cobalamin from protein by converting pepsinogen to the functionally active pepsin. Pepsin is the enzyme responsible for separating protein from vitamin B12. It (pepsin) breaks down proteins into polypeptides.
Vitamin B12 must seperate from protein before binding to IF for transportation to the terminal ileum.
People with achlorhydria don’t make enough stomach acid to release B12 from protein, so they can’t efficiently absorb the vitamin in the ileum.
Pernicious anemia is an autoimmune disease
Lack of Intrinsic Factor (IF) in pernicious is due to autoimmune atrophic gastritis. The condition occurs when antibodies attack and damage the parietal or oxyntic cells of the gastric mucosa that produce IF and gastric acid (hydrochloric acid).
Note that achlorhydria (lack of stomach HCl) is often associated with lack of Intrinsic Factor, and both are often involved together in the development (etiology) of pernicious anemia.
A note to our readers
We strongly recommend that you consult your doctor if you believe you have the symptoms of vitamin B12 deficiency or pernicious anemia. Although the information contained in this article is based on peer-reviewed research, it is meant only to keep you well-informed about issues relating to your health and wellbeing and not in place of advice and care by a qualified medical professional.
Vitamin B12 deficiency and pernicious anemia are potentially life-threatening, so don’t delay seeing your doctor if you believe you have the signs and symptoms of these conditions. Only a qualified medical practitioner can determine the actual cause of your symptoms.

